Article
The Risks of Premature Discharge from the ED
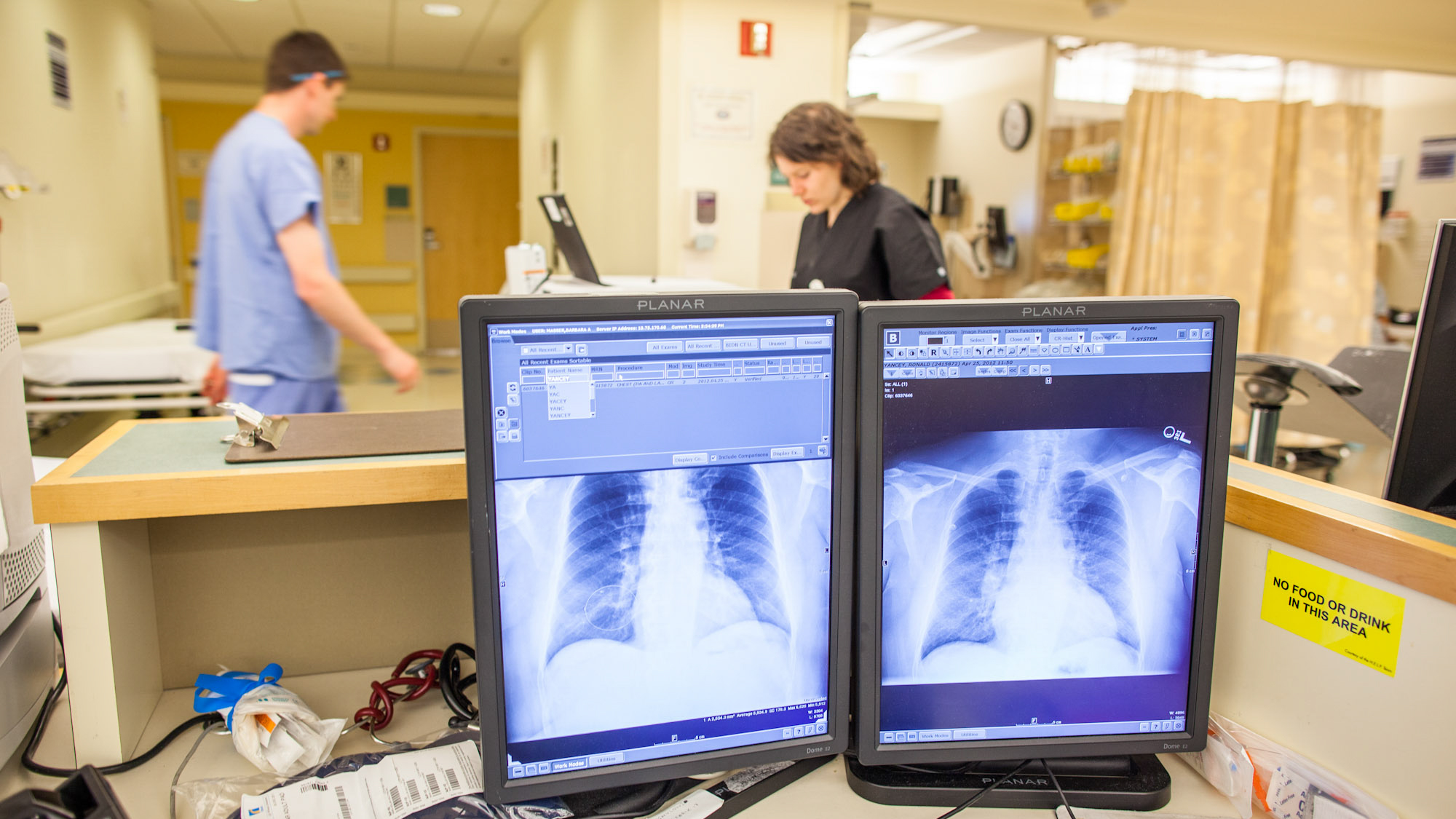
In a service area where diagnostic ambiguity is more the rule than the exception, the physicians and nurses discharging patients rarely hear the end of the patient’s story. For Emergency Medicine physicians—the inevitable sending of a patient home, to an inpatient service, or to a PCP—generally limits meaningful feedback about the accuracy of their diagnosis and treatment plan. Are you concerned about any of these potential risks in your ED?
- test results received in the ED post-discharge
- incomplete or unspecific discharge or follow-up instructions
- patient’s (or family’s) incomplete comprehension of instructions
- patient’s PCP unaware of ED visit and/or need for follow up
- discharge accelerated due to ED production pressure
- discharge without reconciliation of concerning symptoms or test results
- patient abandoned between ED discharge and inpatient admission (i.e., boarders)
Without formal and consistent direct feedback, ED physicians have to contend with a certain amount of anxiety about these and other post-encounter risks—and where to focus patient safety attention and resources.
Systematic input from the patient population, the primary care community, and hospital-based departments can provide ED leaders with a realtime understanding of strengths and weaknesses in the ED’s discharge process. Combining that insight with aggregated, comparative analysis of deeply coded malpractice claims from Candello opens a window into your most critical vulnerabilities.

Case Example: Discharge
A 30-year-old female presented to the ED with history of severe,bilateral lower abdominal pain with nausea and vomiting over the previous three days. Medical record documentation revealed a limited abdominal exam with findings of possible supra pubic pain and no abdominal tenderness. There was no documentation of any abdominal rebounding, or tenderness to the kidney area. No gynecological exam was performed. Labs, urinalysis, and blood cultures revealed possible UTI: white and red blood cells in the urine and elevated white blood cell count with left shift (but specimen contamination was suspected). An abdominal X-ray was negative. The patient was diagnosed with a UTI, prescribed antibiotics, and discharged—despite a 102.3 temperature and no resolution of her abdominal pain or a Urology consult for possible kidney infection.
Two days later, urine cultures returned “no growth,” confirming specimen contamination, and invalidating the diagnosis of a UTI. That same day, the patient was admitted with a ruptured appendix.(Case settled: $50K)
This page is an excerpt of the full Candello report: Malpractice Risks in the Emergency Department.
ED Benchmarking Report Landing Page

